Acoustic Neuromas | Ear and Facial Nerve Tumors | Otosclerosis | Glomus Tumors
Mastoidectomy | Stapedectomy Perforation | Eustachian Tube dilation
Eardrum Perforation
Perforation of the eardrum may have multiple different causes. It can be caused by ear infection, trauma, or less commonly as a sequella of ear tube insertion. There are two main reasons to close a hole in the eardrum. The first is that water exposure through the perforation places bacteria into the middle ear. An ear infection of the middle ear space will usually result. Recurrent infections can lead to mastoiditis bone ear infections. The other reason for closing and patching a perforation is that skin from the outer side of the eardrum “dry skin” can abnormally grow through the perforation into the middle ear space behind the eardrum “wet skin”. The result is that the dry skin builds-up in the area behind the eardrum and will give rise to recurrent ear infection. This is known as “cholesteatoma”. To prevent recurrent ear infections from water exposure and skin growth (cholesteatoma), the perforation is best closed. The closure is known as “tympanoplasty” and is usually performed with a microscope through the ear canal as an outpatient.
Earbone Reconstruction
Chronic otitis media ear infections and tumors can cause damage or destruction of the middle ear bones. In that case, the surgeon can either recommend a hearing aid or reconstruction of the ear bones. Hearing aids work well, but may need maintenance and battery changes. Reconstruction surgery of the ear bones can be very favorable and lead to maintenance-free improved hearing for the patient.
In performing an ossicular bone reconstruction, the surgeon usually works through the ear canal. A microscope is used during the surgery. The microscopically-small bones are palpated and checked. If they are seen to be deficient, they can often be re-worked with micro-drills and replaced into the ear. Sometimes prosthetic devices are used to substitute for the absent the bones. Once the ear bone reconstruction reconnects the eardrum with the inner ear, then hearing is again possible. This surgery is known as “tympanoplasty with ossicular reconstruction”. The surgery is usually done as an outpatient procedure. Heavy activity should be avoided for 10 to 14 days after the surgery procedure.
Cochlear Implants
Dr. Fritsch is a member of the ANA (American Neurotology Society) honorary society.
Cochlear Implantation (CI) has developed into a highly effective means of replacing cochlear function for deaf patients. It is indicated for patients with bilateral, profound, sensorineural hearing loss who make a little or no use of their hearing aids. Children from 6 months up to elderly patients in their late 80’s, have all been implanted. Some patients have challenging anatomical cochlear and inner ear deformities which are accommodated by use of different techniques of surgery. Overall, cochlear implants have helped many patients, with profound sensorineural hearing loss.
The Cochlear Implant device has two parts. There is a subcutaneously implanted device called the “receiver-stimulator”. This device receives signals from external to the head, and relays electrical impulses to the remaining nerves of the inner ear. Externally, the second part of the device is known as the “speech processor”, and resembles a hearing aid. It’s function is to use a microphone to receive speech sound and to process it with a computer microchip into electrical signals. The processor sends the electronic signals through the skin “transcutaneously” to the receiver-stimulator. Thus, the speech sound energy that hits the processor microphone is encoded and sent through the skin via electromagnetic induction signals to the receiver-stimulator. The receiver-stimulator is connected to the inner ear nerve cells which receive the signals and pass them to the brain. The patient learns to interpret the signals as usable speech.
The perceived cochlear implant sound is not the same as natural hearing. The reason for this is that the thousands of cells associated with normal hearing are condensed down to about 20 electrode “cells”. Therefore, the fidelity of the cochlear implant is much less than a natural human ear. Nevertheless, speech can be heard and interaction can take place such that an external observer can hardly tell the difference between a normal hearing patient and a cochlear implant patient. Oftentimes, television and phone usage are possible.
For children who have never heard noise before, learning speech is a long process, just as any learning of a new language would be. For adults who already know language and speech, it is a straight-forward and relatively quick process.
BAHA (Bone Anchored Hearing Aid)
The BAHA device was designed for patients with sensorineural or conductive hearing loss. The advantage is that the aid is a placed in a small area behind the ear and it is camouflaged within the hairline. The bone anchored hearing aid can give very clear hearing for patients who have a conductive hearing loss. For those with sensorineural hearing loss on one side, the sound will be transmitted by the skull to the other side ear allowing the patient to hear sounds well from both sides of the head.
The bone anchored hearing aid is an osteo-integrated screw device, similar to dental implants, that is placed in the bone behind the ear. There is a small exposed post above and behind the ear to which a hearing aid is clipped. The hearing aid will then vibrate the post, which transmits this vibration to the skull and to the inner ear. The clarity is usually excellent for patients with a BAHA.
The surgery for the BAHA can be performed in either one or two stages. Dr. Fritsch generally uses the one stage procedure. This causes less trauma and avoids repetitive surgery.
After the surgery, there is a period of healing period, of the skin around the post. This can take two to three weeks. During this time period, the area must be kept dry. The hair is washed and shampooed over a sink with the area behind the operated ear staying dry. After the three week period, shampooing can take place normally. The key for the BAHA is that after shampooing it is dried and the post is cleaned.
After the surgery, a four month bone healing period, for the screw to osteo-integrate with the bone is required. If the bone has not grown into the implant, then it can slowly vibrate loose from use.
BAHA devices can also be used on both ears. This is commonly done for patients with congenital problems of development for both ears. Sometimes reconstructive surgery cannot be performed for the patient and the BAHA is an excellent alternative for these patients. The BAHA device has been commonly in use for at least ten years.
There are two other devices which have appeared recently. One is known as the Optima Ponto system which is very similar to the BAHA system. Another completely different strategy is a new device known as the Sophono. The Sophono device has a buried device then the hearing aid is held on to the device with a magnet transcutaneously. It offers the great advantages that there is no post exposed and, therefore, no special cleaning is needed.
Acoustic Neuroma (Vestibular Schwannoma)
Dr. Fritsch is a member of the ANA (Acoustic Neuroma Association).
Acoustic neuroma, also known as acoustic schwannoma, vestibular schwannoma, is a benign intracranial tumor forming on the VIII cranial nerve. The VIII cranial nerve is specifically the balance and hearing nerve. These tumors most commonly originate from the vestibular (balance) portion of the VIII nerve from the Schwann cells. The Schwann cells are part of the external covering of nerve. This type of Schwann tumor is generally slow growing, but puts pressure on surrounding structures intra-cranially.
The prevalence of acoustic neuroma is approximately one per 100,000 people. There are approximately 3,000 new acoustic neuromas diagnosed each year within the United States and it compromises approximately 7% of all intracranial tumors in adults. The peak incidents are in the fifth to sixth decades and both sexes are equally affected.
The signs and symptoms of acoustic neuroma are overwhelmingly those of ringing (tinnitus) of the ear and sensori-neural nerve type hearing loss. Small tumors start with these symptoms and larger tumors then progress to numbness in the face, facial nerve twitching or paralysis, as well as problems with swallowing and gag reflexes. Very large tumors may lead to increased intracranial pressure with headache, vomiting, and altered consciousness.
Causes of acoustic neuroma are not generally known and they occur only sporadically within the general population. There is, however, a related tumor is known as Neurofibromatosis II and bilateral acoustic neuromas are very commonly seen and it is a hereditary familial problem. There are multiple other types of tumors which these patients may also have.
Diagnosis:
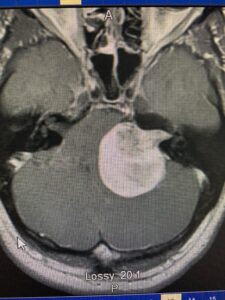
Diagnosis of acoustic neuromas initially begins with a history and physical examination, followed by otologic testing, and finally radiologic scanning. The most commonly used radiological scan is an MRI scan with gadolinium enhancement. On the scan, the tumor can be visualized, as well as its size and its shape.
Treatment:
Acoustic neuromas are generally slow growing tumors. Therefore, many patients are conservatively treated by an observation period. During the observation period, MRI scans are followed to estimate size progression. Many times patients in their elderly years or who are medically infirm will follow this route. Since the growth rate of an acoustic neuroma varies from tumor to tumor, close monitoring is necessary. In a younger person, it is generally known that an observation period will eventually lead to definite treatment, because even a slow-growing tumor will usually enlarge during their lifetime to an unacceptable size.
Surgery:
There are three main surgery directions a surgeon may take to access the tumor. The route specifically taken for any individual depends on the patient’s age, health, and the size and shape of the tumor. Of the three surgical approaches, the most commonly used is the suboccipital approach. In this case, the tumor is approached from behind the ear. An other approach is the translabyrinthine approach, which goes directly through the ear and destroys the ear. It may be indicated if there is no hearing in the patient’s ear and, therefore, nothing to lose by drilling through the ear. The third approach is by the middle cranial fossa, which is reserved for small tumors on the lateral portion of the nerve. The suboccipital approach is very well tolerated and gives wide exposure of the tumor and can be used for all sizes of the tumors. It is generally a team approach between Otologist and Neurosurgeon.
The surgery risks for removal of the acoustic neuroma revolve mainly around the preservation of the facial nerve. In very small tumors, hearing may be preserved. The balance nerves on the affected side are resected with the tumor. The patient also must be aware that it is an intracranial procedure with attendant risks. There is a short intensive care unit stay after the surgery to monitor the patient.
Radiation:
Alternative treatment is Radiation Therapy. This is generally by Gamma-knife radiosurgery or Cyber-knife. The downsides for radiation therapy are induction of other tumors (such as glioblastoma) in the nearby irradiated tissue. As well, the swelling of the tumor may give rise to hearing loss and facial nerve problems. The radiation therapy is often times reserved for patients who are medically infirm and are not able to tolerate surgery. Additionally, long-term scanning is needed after radiation therapy since it does not kill the tumor, but generally “stuns” it. Progression of growth may occur followed by a surgical resection.
Overall, treatment for acoustic neuromas has progressed through specific, but well recognized treatment algorithms. The tumor resection is a common surgery for to physicians who specialize in Otology-Neurotology.
Eustachian Tube dysfunction/Serous Otitis Media ear infections/Ventilation tubes/Pediatric Otitis
Most children will finally outgrow the need for treatment. Between the ages of 5 and 8 years, the head and Eustachian tube growth, as well as the musculature changes, result in a size that allows for the Eustachian tube to become an active passage for air during this time. Ear tubes are then not further needed. The tubes allow children to reach this stage without major ear infection complications.
Treatment:
The mainstay of treatment of otitis media is antibiotics. If four or more episodes of otitis media occur within a year, then ear ventilating tubes are definitely recommended. Some patients receive ear tubes after one infection and include patients who have a cleft palate, those with strong family histories, or those who have significant allergies. Thus, the medical strategy is to treat the Eustachian tube problems and ear infections by antibiotics and tubes until the Eustachian tubes open on their own. This usually happens between the ages of 5 to 8 years. It is very important to treat the ear infections and Eustachian tube dysfunction to prevent other more serious problems such as mastoiditis and cholesteatoma.
There are some special Eustachian tube cases, such as patients who have had irradiation for tumors in the ear area. In these cases, the nasopharynx, which is the area in the back of the throat, may be congested and scarred and impair Eustachian tube function. Such patients often need a lifelong tympanostomy ear tube insertion to substitute for the function of the Eustachian tube.
Ventilating ear tubes:
The tympanostomy ear tube insertion surgery is an excellent method of dealing with Eustachian tube dysfunction because it bypasses the Eustachian tube problems and works 24 hours a day. It ventilates the middle ear space by placing a microscopic hole in the eardrum and then placing a small hollow plastic tube into the hole to hold it open. Since the tube is hollow, it allows ventilation through the ear canal rather than through the Eustachian tube.
The two main types of tubes are temporary and semi-permanent. The temporary tube lasts approximately six months, and the semi-permanent “T-tube” lasts for approximately three to five years. Most children receive a temporary ear tube first since most children need only one application of tubes before the ear mucous-membrane heals itself. Once this temporary tube has extruded, if there is recurrence, then a semi-permanent T-tube is inserted. Some patients, such as cleft plate patients, may start with a semi-permanent tube because they have long-term problems.
Adenoids:
The role of Eustachian tube dysfunction caused by adenoid hypertrophy is controversial. It appears that some patients’ adenoids are highly obstructive of nasal breathing and cause constant mouth-breathing and some of the obstructive adenoids may also cause Eustachian tube dysfunction. However, the incidence of adenoid hypertrophy causing Eustachian tube dysfunction is not truly known.
Otosclerosis/Stapedectomy
Dr. Fritsch is a member of the OSG (Otosclerosis Study group) honorary society.
Otosclerosis (or otospongiosis) is a condition in which motion of the third bone of the ear, the stapes bone, becomes impaired. The stapes bone usually acts as a piston to transfer the vibration of the eardrum to the inner ear. When this piston mechanism is not working properly, hearing is lost. The piston action can no longer work during otosclerosis when the cylinder-like sides of the oval window and the piston-like stapes bone become fused together. The fused bone then results in a “conductive” hearing loss. Conductive hearing loss means that the bones or the eardrum are having problems. Otosclerosis causes the stapes bone to lose function and results in a conductive hearing loss.
Treatment:
The treatment for otosclerosis involves either amplifying sound with a hearing aid or surgically replacing the stapes bone. Treatment with a hearing aid overcomes the problem by amplifying the sound beyond what has been lost due to the impaired stapes bone. Patients with conductive hearing losses, such as otosclerosis, have excellent understanding with a hearing aid. The reason is that the underlying nerve function is normal. Treatment by stapedectomy surgery overcomes the problem by replacing the impaired stapes bone. The surgery is done through the ear canal with a microscope and micro-instruments. A small .5mm hole is laser drilled into the stapes bone footplate. Thereafter, an artificial prosthesis is placed into the small hole to replace of the actual bone. This surgery has been successfully performed by Otologists on a regular basis since the 1960’s. Regular activities including air flight and scuba-diving may be done after the surgery. The surgery is usually performed as an outpatient. To allow for healing, there is no lifting for at least ten days.
Mastoiditis/Cholesteatoma/Mastoidectomy
Dr. Fritsch is a member of the AOS (American Otological Society) honorary society.
The bone immediately behind the external ear is known as the “mastoid bone”. This bone can be felt behind the ear and is the area without hair growing from it. The mastoid bone is configured very similar to a sponge made out of bone. Since the air cells in the bony sponge need to be aerated through the Eustachian tube “pop the ear,” any blockage of the Eustachian tube or the air tract within the mastoid bone can give rise to acute and chronic infected collections within the bone. Those collections then need to be removed in order to stop the ear infection process.
There is a special type of mastoid ear bone infection known as cholesteatoma. In this case, the bone has a problem with skin from the ear canal having grown through an eardrum perforation hole and into the mastoid bone. This gives rise to chronic ear infection drainage and loss of hearing.
All the types of mastoiditis are treated with an operation known as mastoidectomy. An incision is made behind the ear where the ear connects with the head. Through this incision, specialized drills and a microscope are used to remove all infected mastoid bone material. This includes the cholesteatoma, if present. Once all the ear infection has been removed, the surgeon will decide whether the ear is appropriate for an ear bone reconstruction at the time of mastoidectomy. Sometimes, a “second-look” is needed four to six months later. The second-look allows the ear to heal and scar tissue to mature prior to reconstruction placing the small ear bones. If they are placed too soon, then they may not heal correctly and result in some hearing loss.
Even with microscopic removal of the cholesteatoma, there is a rate of recurrence of approximately 10%. Children, in particular, have aggressive acting cholesteatomas and may indeed need further surgery to remove the cholesteatoma and improve the mastoid condition.
In aggressive mastoiditis or cholesteatoma cases, a “canal-wall-down” mastoidectomy procedure may be needed. In this case, the natural configuration of the ear canal is removed and the mastoid is opened to the ear canal. From the outside, this is not really appreciated, but using a speculum and looking through the ear canal a physician can determine that a canal-wall-down procedure has been performed. The reason a mastoid canal-wall-down procedure is performed is to limit the space where cholesteatoma or mastoiditis could reside. Therefore, the recurrence rates are lowered.
A disadvantage of the canal-wall-down mastoidectomy is that the natural ossicular chain is usually disrupted by this operation. Thus, it is a balance between removing the underlying progressive disease and sacrificing hearing function. The hearing function can either be recreated through hearing aid usage or by an ear bone ossicular reconstruction.
Meniere's Syndrome (Meniere's Disease, Endolymphatic Hydrops)
Dr. Fritsch is a member of the ANS (American Neurotology Society) honorary society.
Meniere’s disease consists of a triad of fluctuating hearing loss, tinnitus (ringing), and vertigo. Some patients also have ear “pressure-pain” sensations. These symptoms will occur episodically together or separately. Each patient’s symptoms vary somewhat differently in severity. Unfortunately, the vertigo symptom can become incapacitating.
Causes:
The cause of Meniere’s disease is not completely known. Meniere’s disease rarely occurs in children, but usually begins in both men and women in early middle-age. It appears to be due to an increase of the inner ear fluid pressures. It is not known if this is from lack of resorption or too much fluid production. It appears that the excess fluid pressure within the inner ear causes periodic rupture of some inner ear membranes. This leads to the troubling episodes of vertigo and hearing loss. Most patients with Meniere’s have certain trigger substances. These are known to be sodium intake, caffeine, tobacco, alcohol, and also stress. Sodium intake is the main trigger. Dietary modification of the “triggers” result in 80% of patients having relief of symptoms. Additionally, some patients with Meniere’s disease have an autoimmune disorder of the body where the patient’s own body attacks the inner ear. These patients need medicinal treatments.
Overall, for the 20% of patients who do not respond to dietary and medical treatment, then a surgical procedure may be necessary to help them with their vertigo symptoms.
There are many other causes of dizziness such as cardiovascular, neurologic, and microvascular ischemia (hardening of the arteries). These diagnoses are usually ruled-out by the family doctor prior to sending the patient to see the Otologist ear doctor.
The diagnosis of Meniere’s disease usually depends on a careful history of the symptoms. Comprehensive testing may be used in order to confirm the impression. The hearing test (audiogram) is a major part of that and sometimes also MRI scanning. Other tests such as ENG (electronystagmography balance test), electrocochleography (ECOG), auditory brainstem response testing (ABR/BSER), and lab tests may be needed.
Treatment:
Dietary:
The mainstay of all Meniere’s treatment is initially dietary. Salt (sodium) intake is of primary importance. Most patients start with a 2 gram sodium diet per day. Most American consume over 5 grams of sodium per day. Patients keep track of everything they eat for several days, and then go to the bookstore and buy a sodium guide. The foods are listed with the sodium content. Thus, a banana may have 8 mg and a Big Mac may have 1,500 mg. Once the total intake is known, then the patient knows that they have cut back to appropriate levels of 2,000 mg (2 grams). Usually, within several weeks this diet will cause 80% of patients to remit from their Meniere’s vertigo symptoms.
Outside of the dietary restriction, tobacco, alcohol, and stress may give rise to Meniere’s symptoms. Therefore, these should be monitored and modified.
Medications:
Most medications generally do not directly benefit the Meniere’s patients other than covering the symptoms. Medicines such a Meclizine and Diazepam are these types of medications. Sometimes diuretics like Dyazide (triamterene) are used. In some cases, a steroid is used.
Surgery:
There are three main types of surgery to treat Meniere’s. The surgeon starts with the most conservative surgery to try to help the patient. If the initial procedure does not perform well for the patient, then escalation of surgery types may be needed to remove the disabling vertigo. Endolymphatic-mastoid shunt procedure is the most conservative and is done as an out-patient. Vestibular neurectomy nerve clip is intracranial and is an in-patient procedure. Labyrinthectomy removes all ear components and is an in-patient surgery. Each procedure has different indications.
